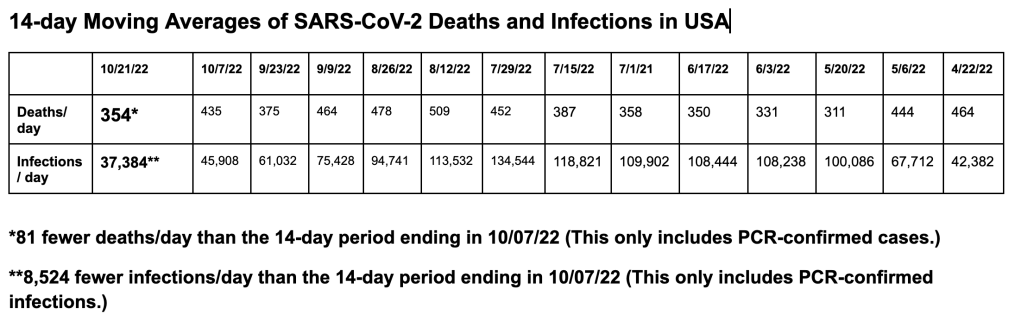
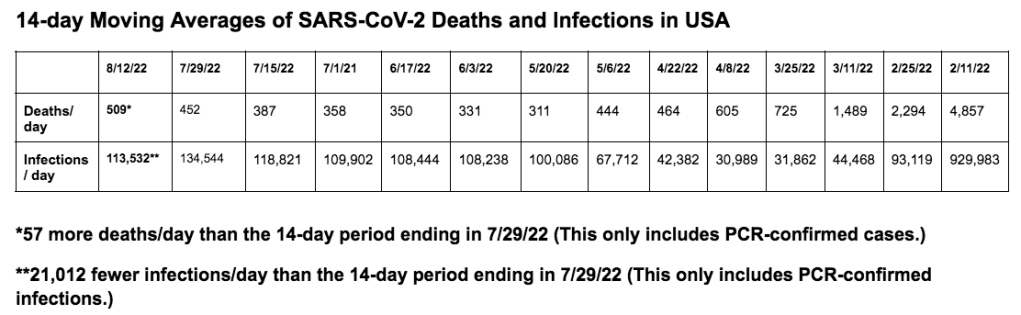
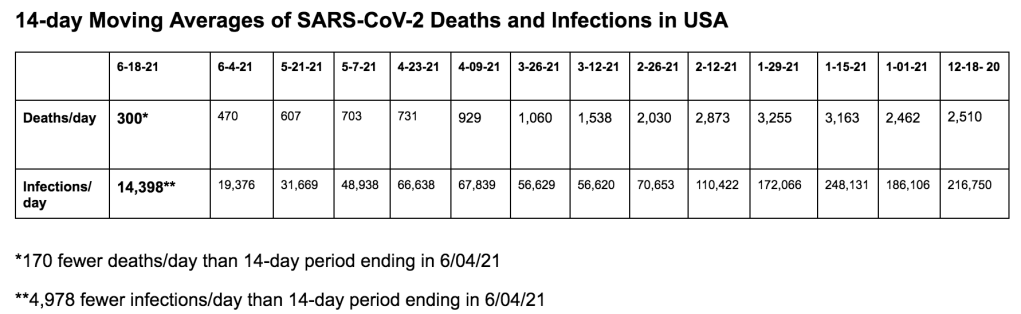
It’s time for our next 14-day moving average determinations for SARS-CoV-2 for the United States and my thoughts on vaccines, SARS-CoV-2 therapeutic agents and mutant viruses. We use the WORLDOMETERS aggregators data set to make any projections since it includes data from the Department of Veterans Affairs, the U.S. Military, federal prisons and the Navajo Nation.

SARS-CoV-2 infections per day in the United States have increased for the first time in 14 weeks. There is still widespread underreporting by states, a failure to capture positive home tests, and a decreased PCR screening program in most states. Deaths per day in the United States have increased by 34 deaths per day. Many states are not reporting deaths or infections in a timely manner. The number of infections per day has increased by 1,683. The CDC estimates that BA.5 accounted for 39.2% (a 23% drop from 10/21/22), BQ.1 accounted for 16.5% (a 7.1% increase since 10/21/22), BQ.1.1 accounted for 18.8% (a 11.6% increase since 10/21/22), BA.4.6 accounted for 9.5%, BF.7 accounted for 9%, BA.2.75.2 accounted for 1.3%, and BA.4 accounted for 0.2%. In the week ending November 5, 2022 BQ isolates accounted for 35.3% of infections. BQ.1.1 has five spike mutations that are different from BA.5. Four of these mutations allow escape from immunity from monoclonal antibodies, any prior infection (including BA.5), or any vaccine to include a BA.5 vaccine.
The total percentage of BQ variant infections in the region that includes New York and New Jersey was 28.4% two weeks ago and is now 52.3%. BA.5.2.6 isolates now account for 3.1% of cases. The BA.2.75 lineages account for 4.2%.
The total percentage of BQ variant infections in the region that includes Pennsylvania, Delaware, Maryland, West Virginia, and Virginia was 17.8% two weeks ago and is now 36.6%. BA.5.2.6 isolates now account for 3.4% of cases. The BA.2.75 lineages account for 3% of cases.
The total percentage of BQ variant infections in the region that includes California, Nevada, Arizona, and Hawaii was 13.6% two weeks ago and is now 36.9%. BA.5.2.6 isolates now account for 2.4% of cases. The BA.2.75 lineages account for 4.2%.
Data on the rapid spread of a dangerous variant category, the BQ variants, was withheld by the CDC in their weekly reports until three weeks ago. The data on BQ.1 and BQ.1.1, the last being a variant with five significant spike protein mutations leading to escape from immunity from prior infections or vaccination. In addition, our monoclonal antibody therapies do not work for these isolates. Infections and hospitalizations in New York are rapidly increasing, secondary to BQ variants. BQ variants have been found in all 10 regions in the United States. Since New York has been a harbinger of things to come throughout the pandemic, we expect the pattern of increased infections, hospitalizations and deaths to continue in many states. These emerging BQ variants are descendants of BA.5. It’s troubling that, despite the availability of a BA.5 bivalent SARS-CoV-2 vaccine, few people are getting vaccinated. As of November 2, 2022, the CDC reports that only 26,378,963 people have received the bivalent vaccine. The Pfizer Omicron BA.5 mRNA booster was administered to 16,748,737 people and the Moderna Omicron BA.5 mRNA booster was administered to 9,630,226 people. In total, 26.3 million people (5 years and up) have received the bivalent vaccine. That’s only 11.6% of people who received the primary series and 7.9% of the overall population.
Children under the age of 5 have not been approved to receive either Omicron BA.5 mRNA boosters. Sadly, in children between 0 and 5 years of age only 1.47 million have received at least one dose of any SARS-CoV-2 mRNA vaccine. In the United States, at least 1,332 children have died of COVID-19, and another 74 have died of multisystem inflammatory syndrome (MIS-C). Worldwide, according to UNICEF, over 16,100 children and young adults aged 0-20 have died of COVID-19.
The October 28 UK Health Security Agency Technical Briefing identifies lineages BQ.1, BQ.1.1, XBB, and BF.7 as isolates of concern. Although BA.5 remains the dominant lineage in the UK, the authors explain, “In the most recent week, logistic growth of variants with 1, 2 or 3 convergent and antigenically significant RBD mutations was respectively 23%, 47%, and 66% per week. The category with 3 RBD mutations consisted largely of BQ.1.1 (59%) with the remainder consisting primarily of a mixture of BA.2.75 sub-lineages (29%).”
| Variant | Sublineage of | Spike Mutations | Global Sequences | UK Sequences |
| BF.7 | BA.5.2.1 | R346T | 11,922 | 2,644 |
| BQ.1 | BA.5 | L452RN460KK444T | 2,490 | 3,207 |
| BQ.1.1 | BA.5 | N460KK444TR346T | 2,304(35 countries) | 1,272 |
| BS.1 | BA.2.3.2 | R346TL452RN460KG476S | 79 | 2 |
In Monterey County, as of 11/5/22, 2.6% of 0-4 year-olds and 40.1% of 5-11 year-olds have received the first two doses of vaccine, while 73.4% of 12-17 year-olds have received two doses. Only 54.5% of Monterey County residents have received a third dose of the vaccine. The Monterey County Health Department does not publish data on how many residents have received the new BA.5 bivalent booster vaccine. On June 17, The FDA authorized both the Pfizer and Moderna vaccines for use in children ages 6 months to four years. We believe children under 5 should be vaccinated as soon as possible. All Monterey County residents should get up to date on COVID-19 vaccinations, including the bivalent BA.5 booster, as soon as possible.
On 11/04/22, the United States had 21,312 documented new infections. There were also 148 deaths. Thirty-five states did not report their infections, and 37 states didn’t report their deaths. In the United States the number of hospitalized patients has increased slightly (+2% compared to the previous 14 days) in many areas and was 27,395 on November 5. On 11/05/22 there were 3,146 patients who were seriously or critically ill; that number was 2,707 two weeks ago. The number of critically ill patients has increased by 439 in the last 14 days, while at least 5,432 new deaths occurred. The number of critically ill patients has decreased for the sixth time in thirty 14-day periods. Patients are still dying each day (average 388/day). Two new Omicron variants BQ.1 and BQ.1.1 are causing increased numbers of infections and hospitalizations in New York. BA.4, BA.4.6, BA.5, and BF.7 variants are still causing infections. In Singapore a different Omicron BA.2 variant, XBB, has caused rapidly increasing infections and now has been named a designated variant along with BQ.1 in the October 28 UK Health Security Agency Technical Briefing. Past infections with a BA.1, BA.2 or BA.5 variants will not prevent infections with any of the newer variants.
As of 11/04/22, we have had 1,098,038 deaths and 99,602,478 SARS-CoV-2 infections in the United States. We have had 546,941 new infections in the last 14 days. We are adding an average of 273,348 new infections every seven days. For the pandemic in the United States we are averaging one death for every 90.71 infections or over 11,024 deaths for each one million infections. As of 11/04/22, thirty-eight states have had greater than 500,000 total infections, and 38 states have had greater than 5,000 total deaths. Forty-six states have had greater than 2,000 deaths, and 43 states have greater than 2,000 deaths per million population. Seven states have over 4,000 deaths per million population: Mississippi (4,365), Arizona (4,338), Alabama (4,193), West Virginia (4,202), New Mexico (4,132), Tennessee (4,118), and Arkansas (4,148). . Eighteen states (Alabama, Virginia, Missouri, North Carolina, Indiana, Tennessee, Massachusetts, Ohio, Michigan, Georgia, Illinois, New Jersey, Pennsylvania, Florida, Texas, New York, Arizona and California) have had greater than 20,000 deaths. Eight states have had greater than 40,000 deaths: Florida (82,357 deaths), Texas (91,737 deaths), New York (73,549 deaths), Pennsylvania (47,840 deaths), Georgia (40,696 deaths), Ohio (40,249 deaths) , Illinois (40,058 deaths), and California (96,984 deaths, 20th most deaths in the world).
On 11/20/20, there were 260,331 (cumulative) deaths in the US from SARS-CoV-2. Since 11/20/20 (23 months), there were 830,937 new deaths from SARS-CoV-2. For nineteen of those months, vaccines have been available to all adults. During these nineteen months, 525,939 people have died of SARS-CoV-2 infections. Clearly, a vaccine-only approach is not working anywhere, especially not in the United States. In addition to getting more people vaccinated, most of the hospitalizations and deaths could have been prevented by proper masking (N95 or better), social distancing, and treatment with oral antiviral agents like Paxlovid. We recommend all of these precautions and treatments to every patient in our clinic, and we have only lost one patient to COVID in 2.5 years.
As of 11/04/22, California was ranked 33rd in the USA in infection percentage at 28.73%. In California, 24.76% of the people were infected in the last 20 months. As of 11/06/22, 24 states have had greater than 30% of their population infected. Fifty states have greater than 20% of their population infected.
Worldwide, average deaths per day are 1,637 for the last 14 days, which is a 68 deaths-per-day increase over the previous 14 days. The United States accounts for 23.70% (388 per day) of all deaths per day in the world over the last two weeks. Worldwide infections per day were 346,369. The United States accounts for 11.28% of those infections (or 39,067 infections per day).
FDA-Approved Oral Drug Treatments for SARS-CoV-2
Pfizer has developed PAXLOVID™, an oral reversible inhibitor of C3-like protease of SARS-CoV-2. The drug inhibits this key enzyme that is crucial for virus production. The compound, also called Compound 6 (PF-07321332), is part of the drug combination PAXLOVID™ (PF-07321332; ritonavir), which just successfully completed a Phase 2-3 trial in humans in multiple countries. The preliminary results were announced on 11/5/21 by Pfizer. The results show that 89% of the hospitalizations and deaths were prevented in the drug treatment arm. The drug was administered twice a day for five days. No deaths occurred in the treatment group, and ten deaths occurred in the placebo group. The study was stopped by an independent data safety monitoring board, and the FDA concurred with this decision. Pfizer applied for an Emergency Use Authorization for this drug on 11/15/21. This drug was approved on 12/23/21. We have only been able to obtain PAXLOVID™ for two patients who we successfully treated with this drug obtained from CVS in Salinas (East Alisal Street; phone number 831-424-0026). They were expecting another shipment on 1/28/22. In my opinion, this agent, if more widely available, could markedly alter the course of every coronavirus infection throughout the world.
Merck has developed the oral drug Molnupiravir, which induces RNA mutagenesis by viral RNA-dependent RNA polymerase of SARS-CoV-2 and other viruses. According to Kabinger et al, “Viral RNA-dependent RNA polymerase uses the active form of Molnupiravir, β-D-N4-hydroxycytidine triphosphate, as a substrate instead of cytidine triphosphate or uridine triphosphate. When the RNA-dependent RNA polymerase uses the resulting RNA as a template, β-D-N4-hydroxycytidine triphosphate directs incorporation of either guanine or adenine, leading to mutated (viral) RNA products. Analysis of RNA-dependent RNA polymerase–RNA complexes that contain mutagenesis products has demonstrated that β-D-N4-hydroxycytidine (the active form of Molnupiravir) can form stable base pairs with either guanine or adenine in RNA-dependent RNA polymerase explaining how the polymerase escapes proofreading and synthesizes mutated RNA” (quotation modified for clarity). The results of the phase 3 trial of Molnupiravir were published in the NEJM article “Molnupiravir for Oral Treatment of Covid-19 in Nonhospitalized Patients” by Angélica Jayk Bernal, M.D. et al. (December 16, 2021 DOI: 10.1056/NEJMoa2116044). In this phase 3 study in the Molnupiravir group, 28 patients were hospitalized and one death occurred. In the placebo group, 53 patients were hospitalized and 9 died. Overall, 47% of hospitalizations and deaths were prevented by Molnupiravir. If you do a post hoc analysis and just look at deaths, Molnupiravir would prevent 89% of deaths. An Emergency Use Authorization by the FDA for Molnupiravir was approved on 12/24/21.The dose of Molnupiravir approved is four 200 mg capsules orally twice a day for five days. Diarrhea is reportedly a side effect in two percent of patients. I treated my first patient with Molnupiravir on 1/28/22. Currently more Molnupiravir is available weekly in the United States than PAXLOVID™ (see chart below; data from PHE.gov). Locally Molnupiravir is still available at CVS in Monterey (Fremont Blvd.; phone number: 831-375-5135) and CVS in Salinas (East Alisal Street; phone number 831-424-0026).
28, p740–746 (2021)with four 200 mg capsules orally twice a day for five dayfour 200 mg capsules orally twice a day for five daysIntravenous Drug Treatment for non-hospitalized SARS-CoV-2 Infected Patient
FDA-Approved Intravenous Monoclonal Antibody Treatment for Non-Hospitalized SARS-CoV-2 Patients
Bebtelovimab is a monoclonal antibody treatment for mild-to-moderate COVID-19 in adults and pediatric patients (12 years of age and older weighing at least 40 kg) with positive results of direct SARS-CoV-2 viral testing, and who are at high risk for progression to severe COVID-19, including hospitalization or death, and for whom alternative COVID-19 treatment options approved or authorized by FDA are not accessible or clinically appropriate. The authorized dose of bebtelovimab is 175 mg, given as an intravenous injection over at least 30 seconds. The U.S. Food and Drug Administration (FDA) has issued an Emergency Use Authorization (EUA) for this drug on 2/11/22. Bebtelovimab is a human antibody that demonstrates neutralization against the Omicron variants and is available in every state and many hospitals and some clinics. If you are planning on using a monoclonal antibody to treat a SARS-CoV-2 infection, currently only bebtelovimab has activity against all Omicron variants, including BA.4.6. Researchers at Columbia University recently reported that “The loss of activity of tixagevimab and cilgavimab [components of Evusheld] against BA.4.6 leaves us with bebtelovimab as the only therapeutic mAb that has retained potent activity against all circulating forms of SARS-CoV-2.” For this reason, we no longer recommend Evusheld for immunocompromised patients with Omicron infections.
An examination of the three variants that Wang et al identified as capable of immune escape in patients who receive the two monoclonal antibodies that are contained in Evusheld reveals that all three variants have a mutation in the spike protein at position 346. The changes substitute an uncharged amino acid— threonine (T), serine (S), or isoleucine (I)—for a positively-charged amino acid, arginine. This just goes to show that a single point mutation in the spike protein can render a monoclonal antibody treatment ineffective. Policy makers should keep in mind that the only way to prevent new drug-resistant variants like BA.4.6 from emerging is to prevent transmission of SARS-CoV-2 in the first place, using non-pharmaceutical interventions. The lack of use of N95 masks, with impending winter and influenza outbreaks, on top of COVID-19, is not wise public health and infectious disease policy. If we don’t make effective use of the non-pharmaceutical interventions available to us (masks, ventilation, social distancing), then the pharmaceutical interventions we have will all eventually be useless.
Two virologists collaborated on Twitter to create the figure below, which Professor Johnson titled “Convergent Evolution on Steroids.” It shows the key mutations present in many of the currently-circulating Omicron subvariants and demonstrates that mutation at site 346 is becoming more and more common. This means that even if prevalence of BA.4.6 wanes, we are still likely to have drug resistance issues with other newer variants.
From Daniele Focosi, M.D., Ph.D. @dfocosi on Twitter
Watching World Data
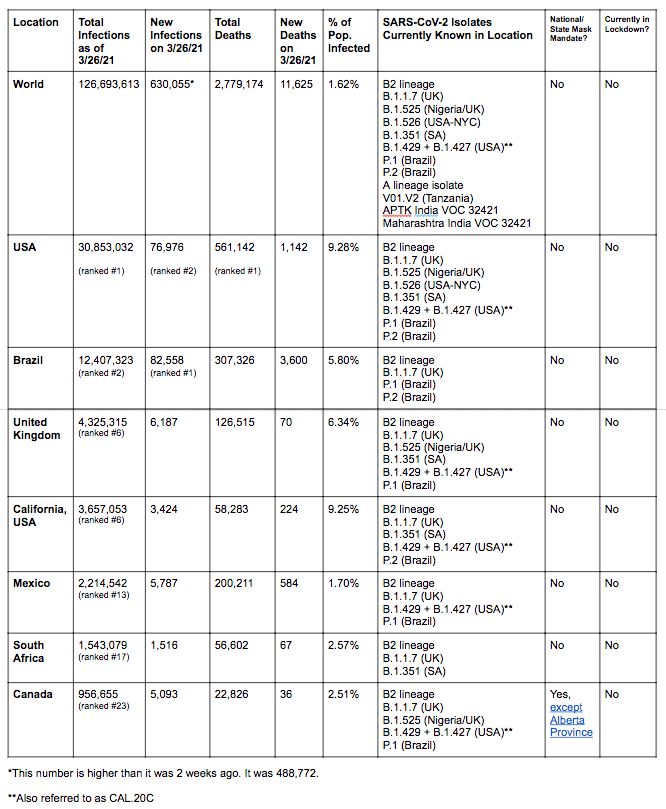
Over the next few months, we’ll be paying close attention to correlations between the SARS-CoV-2 data, the number of isolates identified in various countries and states, and the non-pharmaceutical interventions (like mask mandates and lockdowns) put in place by state and national governments. Data on infections, deaths, and percent of population infected was compiled from Worldometers. Data for this table for SARS-CoV-2 Isolates Currently Known in Location was compiled from GISAID and the CDC. It’s worth noting that GISAID provided more data than the CDC.
| Location | Total Infections as of 11/04/22 | New Infections on 11/04/22 | Total Deaths | New Deaths on 11/04/22 | % of Pop.Infected | SARS-CoV-2 Isolates Currently Known in Location | National/ State Mask Mandate | Currently in Lockdown |
| World | 637,281,842(4,849,164 new infections in 14 days). | 273,333 | 6,604,448(22,918 new deaths in last 14 days) | 1,091 | 8.17% | B2 lineageAlpha/B.1.1.7 (UK)Eta/B.1.525 (Nigeria/UK)Iota/B.1.526 (USA-NYC)Beta/B.1.351 (SA)Epsilon/B.1.427 + B.1.429 (USA)*Gamma/P.1 (Brazil)Zeta/P.2 (Brazil)A lineage isolateV01.V2 (Tanzania)APTK India VOC 32421Delta/B.1.617.2 (India)BV-1 (Texas, USA)Kappa/B.1.617.1 (India)Lambda/C.37 (Peru)Theta/P.3 (Philippines) Mu/B.1.621 (Colombia)C.1.2 (South Africa 2% of isolates in July 2021)R1 (Japan)Omicron/B.1.1.529 + BA.1 + BA.2 + BA.3 (South Africa November 2021)B.1.640.1 (Congo/France)B.1.640.2 (Cameroon/France)Four new recombinants 12/31 to 3/22)BA.2.12.1 (USA)BA.4 (South Africa)BA.5 (South Africa)BA.2.75 (India 7/22)BA.4.6 (USA 7/22)BF.7BJ.1XBBBQ.1BQ.1.1BS.1 | No | No |
| USA | 99,602,478(ranked #1) 546,941 new infections in the last 14 days or 39,067/day. | 19,652(ranked #6) 35 states and D,C. failed to report infections on 11/04/22. | 1,098,038(ranked #1) 5,432 new deaths reported in the last 14 days or 388/day. | 148 37 states and D.C. failed to report deaths on 11/04/22. | 29.74% | B2 lineageAlpha/B.1.1.7 (UK)Eta/B.1.525 (Nigeria/UK)Iota/B.1.526 (USA-NYC)Beta/B.1.351 (SA)Epsilon/B.1.427 + B.1.429 (USA)*Gamma/P.1 (Brazil)Zeta/P.2 (Brazil)Delta/B.1.617.2 (India)BV-1 (Texas, USA)Theta/P.3 (Philippines) Theta/P.3 (Philippines) Kappa/B.1.617.1 (India)Lambda/C.37 (Peru)Mu/B.1.621 (Colombia)R1(Japan) Omicron/B.1.1.529 + BA.1 + BA.2 (South Africa November 2021)B.1.640.1 (Congo/France)Recombinant Delta AY.119.2- Omicron BA.1.1 (Tennessee, USA 12/31/21)\BA.2BA.2.12.1 (United States)BA.4 (South Africa 11/21)BA.5 (South Africa 11/21)BA.2.75 (India 7/22)BA.4.6 (USA 7/22) | No | No |
| Brazil | 34,890,243(ranked #5) 62,069 new infections in the last 14 days. | 2,738 | 688,384(ranked #2; 803 new deaths in 14 days) | 68 | 16.20% | B2 lineageAlpha/B.1.1.7 (UK)Beta/B.1.351 (SA)Gamma/P.1 (Brazil)Zeta/P.2 (Brazil)Lambda/C.37 (Peru)Mu/B.1.621 (Colombia) Omicron/B.1.1.529 + BA.1 (South Africa November 2021)BA.2BA.2.12.1 (United States)BA.4 (South Africa 11/21)BA.5 (South Africa 11/21) | No | No |
| India | 44,659,447(ranked #2); 18,699 new infections in 2 weeks. | 1,082 | 530,486(ranked #3) 1,529 new deaths in 2 weeks. | 7 | 3.17% | B2 lineageAlpha/B.1.1.7 (UK)Beta/B.1.351 (SA)Gamma/P.1 (Brazil)Epsilon/B.1.427 + B.1.429 (USA)*Eta/B.1.525 (Nigeria/UK)APTK India VOI 32421Delta/B.1.617.2 (India)Kappa/B.1.617.1 (India)Iota/B.1.526 (USA-NYC) Omicron/B.1.1.529 + BA.1 (South Africa November 2021)B.1.640.1 (Congo/France)BA.4 (South Africa 11/21)BA.5 (South Africa 11/21)BA.2.75 (India) | No | No |
| United Kingdom | 23,930,041(ranked #7) 74,519 new infections in 2 weeks. | – | 194,704 (ranked #7) 2,022 new deaths in 2 weeks | – | 34.93% | B2 lineageAlpha/B.1.1.7 (UK)Eta/B.1.525 (Nigeria/UK)Beta/B.1.351 (SA)Epsilon/B.1.427 + B.1.429 (USA)*Gamma/P.1 (Brazil)Delta/B.1.617.2 (India)Theta/P.3 (Philippines) Kappa/B.1.617.1 (India)Lambda/C.37 (Peru)Mu/B.1.621 (Colombia)C.1.2 (South Africa)Omicron/B.1.1.529 + BA.1 (South Africa November 2021)B.1.640.1 (Congo/France)XD (AY.4/BA.1) recombinantXF (Delta/BA.1) recombinantXE (BA.1/BA.2) recombinantBA.2BA.2.12.1 (United States)BA.4 (South Africa 11/21)BA.5 (South Africa 11/21)BA.2.75 (India 7/22) | No | No |
| California, USA | 11,353,896(ranked #13 in the world; 21,351 new infections in the last 14 days). | 1,434 | 96,984 (ranked #20 in world) 303 new deaths in the last 14 days | 7 | 28.73% | B2 lineageAlpha/B.1.1.7 (UK)Eta/B.1.525 (Nigeria/UK)Beta/B.1.351 (SA)Gamma/P.1 (Brazil)Epsilon/B.1.427 + B.1.429 (USA)*Zeta/P.2 (Brazil)Delta/B.1.617.2 (India)Theta/P.3 (Philippines) Kappa/B.1.617.1 (India)Lambda/C.37 (Peru) Mu/B.1.621 (Colombia) Omicron/B.1.1.529 + BA.1 (South Africa November 2021)BA.2BA.2.12.1 (United States)BA.4 (South Africa 11/21)BA.5 (South Africa 11/21)BA.2.75 (India 7/22) | No | No |
| Mexico | 7,113,132(ranked #19) 7,114 new infections in 14 days). | 628 | 330,415(ranked #5)94 new deaths in 14 days) | 5 | 5.40% | No | No | |
| South Africa | 4,029,737(ranked #37; 4,362 new infections in 14 days). | 241 | 102,363 (ranked #18) 106 new deaths in 14 days) | 52 | 6.63% | B2 lineageAlpha/B.1.1.7 (UK)Beta/B.1.351 (SA)Delta/B.1.617.2 (India)Kappa/B.1.617.1 (India) C.1.2 (South Africa, July 2021)Omicron/B.1.1.529 + BA.1 (South Africa November 2021)B.1.640.1 (Congo/France)BA.2BA.4 (South Africa 11/21)BA.5 (South Africa 11/21) | No | No |
| Canada | 4,336,860(ranked #33) 22,142 new infections in 14 days). | – | 46,389(ranked #25 ) 364 new deaths in the last 14 days | – | 11.29% | No | No | |
| Poland | 6,333,591 (ranked #21; 9,506 new infections in 14 days). | 693 | 118,157 (ranked #15)142 new deaths in the last 14 days | 14 | 16.80% | B2 lineageAlpha/B.1.1.7 (UK)Eta/B.1.525 (Nigeria/UK)Beta/B.1.351 (SA)Delta/B.1.617.2 (India)Mu/B.1.621 (Colombia)Omicron/B.1.1.529 + BA.1 + (South Africa November 2021),Omicron/B.1.1.529 +BA.3 | No | No |
| Russia | 21,453667(ranked #10), 98,753 new infections in 14 days). | 6,149 (ranked #9) | 390,459(ranked #4)1,100 new deaths in 14 days | 71 | 14.71% | No | No | |
| Peru | 4,159,132(ranked #36, 7,113new infections in 14 days). | 598 | 216,972(ranked #6) 95 new deaths in the last 14 days | 5 | 12.34% | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India)Gamma/P.1 (Brazil)Iota/B.1.526 (USA-NYC)Lambda/C.37 (Peru)Mu/B.1.621 (Colombia)Omicron/B.1.1.529 + BA.1 (South Africa November 2021) | No | No |
| Iran | 7,558,002(ranked #17; 2,308 new infections in last 14 days) | 40 | 144,587(ranked #12) 47 new deaths in the last 14 days | 4 | 8.78% | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India)Beta/B.1.351 (SA)Omicron/B.1.1.529 + BA.1 (South Africa November 2021) | No | No |
| Spain | 13,529,643(ranked #12; 41,628 new infections in 14 days). | 2,551 | 115,239 (ranked #16)381 new deaths in 14 days | 23 | 28.95% | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India)Beta/B.1.351 (SA)Gamma/P.1 (Brazil)Epsilon/B.1.427 + B.1.429 (USA)*Eta/B.1.525 (Nigeria/UK)Iota/B.1.526 (USA-NYC)Kappa/B.1.617.1 (India)Mu/B.1.621 (Colombia)Omicron/B.1.1.529 + BA.1 (South Africa November 2021)B.1.640.1 (Congo/France) | No | No |
| France | 36,920,064 (ranked #3; 395,459 new infections in the last 14 days). | 29,438 (ranked #4) | 157,277 (ranked #10)940 new deaths in 14 days. | 78 | 56.29% a 0.60% increase in 14 days. | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India) Omicron/B.1.1.529 South Africa November 2021)B.1.640.1 (Congo/France)B.1.640.2 (Cameroon/France)GKA (AY.4/BA.1) recombinant | No | No |
| Germany | 35,823,771(ranked #4; 651,078 new infections in 14 days.) | 38,859 (ranked #2) | 154,535 (ranked #11)2,053 new deaths in 14 days | 207 | 42.70% 0.77% increase in 14 days | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India) Delta/B.1.617.2 (India) Omicron/B.1.1.529 South Africa November 2021)GKA (AY.4/BA.1) recombinant | No | No |
| South Korea | 25,760,701 (ranked #6 516,446 new infections in 14 days). | 43,424(ranked #1) | 29,315 (ranked #36) 363 new deaths in 14 days | 35 | 49.18%1.00% increase in 14 days | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India) Delta/B.1.617.2 (India) Omicron/B.1.1.529 South Africa November 2021) | No | No |
| Vietnam | 11,505,249 (ranked #13; 8,895 new infections in 14 days). | 339 | 43,165(ranked #26) | – | 11.62% | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India) Delta/B.1.617.2 (India) Omicron/B.1.1.529 South Africa November 2021) | No | No |
| Netherlands | 8,521,729 (ranked #16; 27,024 new infections in 14 days). | 1,225 | 22,845 (ranked #41) | 3 | 49.51% | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India) Delta/B.1.617.2 (India) Omicron/B.1.1.529 South Africa November 2021)GKA (AY.4/BA.1) recombinant | No | No |
| Denmark | 3,138,750 (ranked #40) 7,601 new infections in 14 days. | 355 | 7,387 (ranked #78 139 new deaths in the last 14 days) | 12 | 53.79% | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India) Delta/B.1.617.2 (India) Omicron/B.1.1.529 South Africa November 2021)GKA (AY.4/BA.1) recombinant | No | No |
| Taiwan | 7,837,658(ranked #17)458,453 new infections in 14 days | 27,594 (ranked #5) | 13,084 (ranked #59 878 new deaths in the last 14 days) | 74 | 32.80% 1.91% of population has been infected in the last 14 days | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India) Delta/B.1.617.2 (India) Omicron/B.1.1.529 South Africa November 2021) | No | No |
| Japan | 22,534,377(ranked #9)608,146 new infections in the last 14 days | 34,064(ranked #5) | 46,898(ranked #24) 757 new deaths in the last 14 days | 59 | 17.94% | B2 lineageAlpha/B.1.1.7 (UK)Delta/B.1.617.2 (India) Delta/B.1.617.2 (India) Omicron/B.1.1.529 South Africa November 2021)BA.2*BA.5* | No | No |
| Argentina | 9,718,875 (ranked #15) | – | 129,991(ranked #14) | – | 21.12% | No | No | |
| Italy | 23,642,011 (ranked #8) | – | 179,436(ranked #8) | 39,23% | No | No | ||
| Chile | 4,777,208(ranked #28) | 7,570 | 61,737(ranked #22) | 12 | 24.81% | No | No | |
| Colombia | 6,310,332(ranked #14) | – | 141,850(ranked #13) | – | 12.25% | No | No | |
| Australia | 9,718,875(ranked #14) | 15,618 (ranked #7) | 15,776(ranked #55) | 59 | 39.95% | No | No | |
| Turkey | 16,919,638(ranked #11) | – | 101,203(ranked #19) | – | 19.77% | No | No | |
| Indonesia | 6,512,913 (ranked #20) | 5,303 (ranked #11) | 158,768 (ranked #9) | 31 | 23,23% | No | No | |
| Malaysia | 4,918,917 (ranked #29) | 4,360 (ranked #13) | 36,481 (ranked #29) | 1 | 14.75% | No | No |
What Our Team Is Reading This Week
- Successful treatment of prolonged, severe COVID-19 lower respiratory tract disease in a B-cell ALL patient with an extended course of remdesivir and nirmatrelvir/ritonavir (Clinical Infectious Diseases) https://doi.org/10.1093/cid/ciac868
- Impact of SARS-CoV-2 ORF6 and its variant polymorphisms on host responses and viral pathogenesis (Preprint) https://doi.org/10.1101/2022.10.18.512708
- Anti-PF4 antibodies associated with disease severity in COVID-19 (PNAS) https://www.pnas.org/doi/10.1073/pnas.2213361119
- A multinational Delphi consensus to end the COVID-19 public health threat (Nature) https://doi.org/10.1038/s41586-022-05398-2
- Pfizer and BioNTech Announce Updated Clinical Data for Omicron BA.4/BA.5-Adapted Bivalent Booster Demonstrating Substantially Higher Immune Response in Adults Compared to the Original COVID-19 Vaccine https://www.pfizer.com/news/press-release/press-release-detail/pfizer-and-biontech-announce-updated-clinical-data-omicron
- Paxlovid and Long Covid (Ground Truths, Eric Topol) https://erictopol.substack.com/p/paxlovid-and-long-covid?utm_source=substack&utm_medium=email
- Risk of Infection and Hospitalization Among Children and Adolescents in New York After Emergence of the SARS-CoV-2 Omicron Variant – Comment and Response (JAMA) https://jamanetwork.com/journals/jama/article-abstract/2797231
- Myocarditis (NEJM) https://www.nejm.org/doi/full/10.1056/NEJMra2114478
- SARS-CoV-2 variants of concern and variants under investigation in England Technical briefing 47 (UK Health Security Agency) https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1115077/Technical-Briefing-47.pdf
- Effectiveness of Monovalent mRNA Vaccines Against COVID-19–Associated Hospitalization Among Immunocompetent Adults During BA.1/BA.2 and BA.4/BA.5 Predominant Periods of SARS-CoV-2 Omicron Variant in the United States — IVY Network, 18 States, December 26, 2021–August 31, 2022 (MMWR) https://www.cdc.gov/mmwr/volumes/71/wr/mm7142a3.htm
- “Three-dose monovalent mRNA VE estimates against COVID-19–associated hospitalization decreased with time since vaccination. Three-dose VE during the BA.1/BA.2 and BA.4/BA.5 periods was 79% and 60%, respectively, during the initial 120 days after the third dose and decreased to 41% and 29%, respectively, after 120 days from vaccination.”
- Saliva antibody-fingerprint of reactivated latent viruses after mild/asymptomatic COVID-19 is unique in patients with myalgic-encephalomyelitis/chronic fatigue syndrome (Frontiers in Immunology) https://doi.org/10.3389/fimmu.2022.949787
- SARS-CoV-2 Nsp6 causes cardiac defects through MGA/MAX complex-mediated increased glycolysis (Preprint) https://doi.org/10.21203/rs.3.rs-1677754/v1
- WHO’s Therapeutics and COVID-19 Living Guideline on mAbs needs to be reassessed (The Lancet) https://www.thelancet.com/journals/lancet/article/PIIS0140-6736(22)01938-9/fulltext
- SARS-CoV-2 disrupts host epigenetic regulation via histone mimicry (Nature) https://doi.org/10.1038/s41586-022-05282-z
- Real-world effectiveness of molnupiravir and nirmatrelvir plus ritonavir against mortality, hospitalisation, and in-hospital outcomes among community-dwelling, ambulatory patients with confirmed SARS-CoV-2 infection during the omicron wave in Hong Kong: an observational study (The Lancet) https://doi.org/10.1016/S0140-6736(22)01586-0
- An ACE2-dependent Sarbecovirus in Russian bats is resistant to SARS-CoV-2 vaccines (PLOS Pathogens) https://doi.org/10.1371/journal.ppat.1010828
- Plasma cytokine levels reveal deficiencies in IL-8 and gamma interferon in Long-COVID (Preprint) https://doi.org/10.1101/2022.10.03.22280661
- Lingering cardiac involvement in previously well people after mild COVID-19 (Nature Medicine) https://www.nature.com/articles/s41591-022-02002-y
- SARS-CoV-2 variants of concern and variants under investigation in England: technical briefing 46 (UK Health Security Agency) https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1109820/Technical-Briefing-46.pdf
- Rapid initiation of nasal saline irrigation to reduce severity in high-risk COVID+ outpatients (Ear, Nose, and Throat Journal) https://doi.org/10.1177/01455613221123737
- SARS-CoV-2 Omicron boosting induces de novo B cell response in humans (Preprint) https://doi.org/10.1101/2022.09.22.509040
- Imprinted SARS-CoV-2 humoral immunity induces converging Omicron RBD evolution (Preprint) https://www.biorxiv.org/content/10.1101/2022.09.15.507787v2
- Note: This is a frightening paper and if the conclusions are accurate humans in general are in trouble. From other papers the facts that HERV-M and EBV are activated by SARS-CoV-2 infection does not bode well for humans moving forward.
- SARS-CoV-2 Omicron boosting induces de novo B cell response in humans (Preprint) https://www.biorxiv.org/content/10.1101/2022.09.22.509040v1
- Evolution of antibody immunity following Omicron BA.1 breakthrough infection (Preprint) https://www.biorxiv.org/content/10.1101/2022.09.21.508922v1
- SARS-CoV-2 Spike protein promotes vWF secretion and thrombosis via endothelial cytoskeleton-associated protein 4 (CKAP4) (Signal Transduction and Targeted Therapy) https://www.nature.com/articles/s41392-022-01183-9
- Long-term neurologic outcomes of COVID-19 (Nature Medicine) https://www.nature.com/articles/s41591-022-02001-z
- Pulmonary Dysfunction after Pediatric COVID-19 (Radiology) https://pubs.rsna.org/doi/10.1148/radiol.221250
- Severe Respiratory Illnesses Associated with Rhinoviruses and/or Enteroviruses Including EV-D68 – Multistate, 2022 (CDC) https://emergency.cdc.gov/han/2022/han00474.asp
- VACCINE INFORMATION FACT SHEET FOR RECIPIENTS AND CAREGIVERS ABOUT COMIRNATY (COVID-19 VACCINE, mRNA), THE PFIZER-BIONTECH COVID-19 VACCINE, AND THE PFIZER-BIONTECH COVID-19 VACCINE BIVALENT (ORIGINAL AND OMICRON BA.4/BA.5) TO PREVENT CORONAVIRUS DISEASE 2019 (COVID-19) FOR USE IN INDIVIDUALS 12 YEARS OF AGE AND OLDER https://labeling.pfizer.com/ShowLabeling.aspx?id=14472
- Pfizer/BioNTech COVID-19 Omicron-Modified Bivalent Vaccine https://www.cdc.gov/vaccines/acip/meetings/downloads/slides-2022-09-01/07-covid-swanson-508.pdf
- Coronavirus (COVID-19) Update: FDA Authorizes Moderna, Pfizer-BioNTech Bivalent COVID-19 Vaccines for Use as a Booster Dose (FDA) https://www.fda.gov/news-events/press-announcements/coronavirus-covid-19-update-fda-authorizes-moderna-pfizer-biontech-bivalent-covid-19-vaccines-use
- Resistance of SARS-CoV-2 Omicron Subvariant BA.4.6 to Antibody Neutralization (Preprint) https://www.biorxiv.org/content/10.1101/2022.09.05.506628v1.full
- SARS-CoV-2 variants of concern and variants under investigation in England Technical briefing 45, 9 September 2022 (UK Health Security Agency) https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1103869/Technical-Briefing-45-9September2022.pdf
- SARS CoV-2 detected in neonatal stool remote from maternal COVID-19 during pregnancy (Pediatric Research) https://doi.org/10.1038/s41390-022-02266-7
- SARS-CoV-2 variants of concern: spike protein mutational analysis and epitope for broad neutralization (Nature Communications) https://doi.org/10.1038/s41467-022-32262-8
- Is SARS-CoV-2 an oncogenic virus? (Journal of Infection) https://doi.org/10.1016/j.jinf.2022.08.005
- Emergence of immune escape at dominant SARS-CoV-2 killer T cell epitope (Cell) https://doi.org/10.1016/j.cell.2022.07.002
- Neurological and psychiatric risk trajectories after SARS-CoV-2 infection: an analysis of 2-year retrospective cohort studies including 1 284 437 patients (The Lancet Psychiatry) https://doi.org/10.1016/S2215-0366(22)00260-7
- An Antibody from Single Human VH-rearranging Mouse Neutralizes All SARS-CoV-2 Variants Through BA.5 by Inhibiting Membrane Fusion (Science Immunology) https://doi.org/10.1126/sciimmunol.add5446
- Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS) is common in post-acute sequelae of SARS-CoV-2 infection (PASC): Results from a post-COVID-19 multidisciplinary clinic (Preprint) https://doi.org/10.1101/2022.08.03.22278363
- Evaluation of publication bias for 12 clinical trials of molnupiravir to treat SARS-CoV-2 infection in 13,694 patients (Preprint) https://www.researchsquare.com/article/rs-1913200/v1
- Anti-neuronal antibodies against brainstem antigens are associated with COVID-19 (eBioMedicine) https://doi.org/10.1016/j.ebiom.2022.104211
- Risk of SARS-CoV-2 Acquisition in Health Care Workers According to Cumulative Patient Exposure and Preferred Mask Type (JAMA Infectious Diseases) http://jamanetwork.com/article.aspx?doi=10.1001/jamanetworkopen.2022.26816
- Coronavirus spike protein activated natural immune response, damaged heart muscle cells (AHA Basic Cardiovascular Sciences Meeting) https://newsroom.heart.org/news/coronavirus-spike-protein-activated-natural-immune-response-damaged-heart-muscle-cells
- Distinguishing features of Long COVID identified through immune profiling (Preprint) https://doi.org/10.1101/2022.08.09.22278592
- Virological characteristics of the SARS-CoV-2 Omicron BA.2.75 (Preprint) https://doi.org/10.1101/2022.08.07.503115
- Multiple pathways for SARS-CoV-2 resistance to nirmatrelvir (Preprint) https://doi.org/10.1101/2022.08.07.499047
- Transmissible SARS-CoV-2 variants with resistance to clinical protease inhibitors (Preprint) https://doi.org/10.1101/2022.08.07.503099
- Comparative pathogenicity of SARS-CoV-2 Omicron subvariants including BA.1, BA.2, and BA.5 (Preprint) https://doi.org/10.1101/2022.08.05.502758
- Neuropathology and virus in brain of SARS-CoV-2 infected non-human primates (Nature Communications) https://doi.org/10.1038/s41467-022-29440-z
- SARS-CoV-2 Brain Regional Detection, Histopathology, Gene Expression, and Immunomodulatory Changes in Decedents with COVID-19 (Journal of Neuropathology and Experimental Neurology) https://doi.org/10.1093/jnen/nlac056
- Examination of SARS-CoV-2 In-Class Transmission at a Large Urban University With Public Health Mandates Using Epidemiological and Genomic Methodology (JAMA) http://jamanetwork.com/article.aspx?doi=10.1001/jamanetworkopen.2022.25430
- Antiviral treatment is more effective than smallpox vaccination upon lethal monkeypox virus infection (Nature) https://doi.org/10.1038/nature04295
- Impact of Pre-Existing Chronic Viral Infection and Reactivation on the Development of Long COVID (Preprint) https://doi.org/10.1101/2022.06.21.22276660
- Notes from the Field: Increase in Pediatric Intracranial Infections During the COVID-19 Pandemic — Eight Pediatric Hospitals, United States, March 2020–March 2022 (MMWR) http://dx.doi.org/10.15585/mmwr.mm7131a4
- Broadly neutralizing antibodies target the coronavirus fusion peptide (Science) https://doi.org/10.1126/science.abq3773
- Efficacy and Safety of a Recombinant Plant-Based Adjuvanted Covid-19 Vaccine (NEJM) https://www.nejm.org/doi/full/10.1056/NEJMoa2201300
- Efficacy and Safety of the RBD-Dimer–Based Covid-19 Vaccine ZF2001 in Adults (NEJM) https://www.nejm.org/doi/full/10.1056/NEJMoa2202261
















You must be logged in to post a comment.