In 2022, multiple new Omicron variants BA.1, BA.2, BA.4, and BA.5 assaulted the world’s population of humans and other animals. By the time multiple companies made and tested Omicron BA.1 vaccines, BA.1 was no longer the dominant variant; in fact, it was no longer present. On August 31, 2022, the FDA allowed rapid introduction of an Omicron BA.5 bivalent vaccine. In 2023 our problems are being caused by XBB recombinant variants and BA.5 sub-variants BQ.1 and BQ.1.1. The Omicron BA.5 bivalent vaccine has had no effect on the immune evading BQ variants or XBB recombinant variants. In December the first highly infectious recombinant variant, XBB, began spreading around the world. The XBB variant XBB.1.5, has rapidly spread across the country and the world. Another new variant, CH.1.1 (BA.2.75.3.4.1.1.1.1) caused 5.9% of infections in the world from December 25 to January 14, 2023 and, from December 26 to January 1, 19.5% of infections in the United Kingdom.
On January 13, the World Health Organization (WHO) updated its recommendations on mask wearing to specify that, given the global spread of COVID-19, masks should be worn “irrespective of the local epidemiological situation,” meaning that masks are now recommended for everyone, not just people in areas with high levels of transmission.
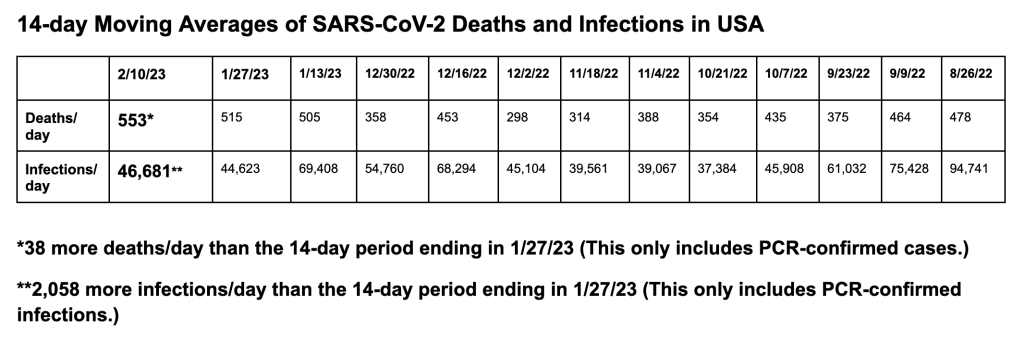
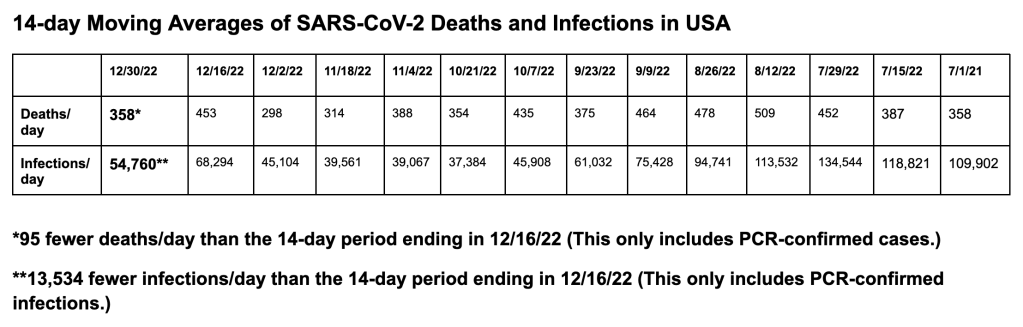
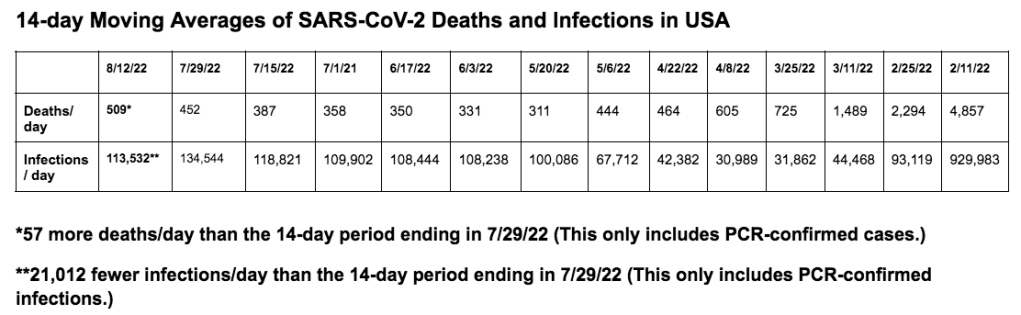
Here are our 14-day moving average determinations for SARS-CoV-2 for the United States. We use the WORLDOMETERS aggregators data set to make any projections since it includes data from the Department of Veterans Affairs, the U.S. Military, federal prisons and the Navajo Nation.
XBB.1.5 Variant Continues to Dominate in the United States
During the week ending in 2/11/23, the CDC estimates that based on genomic surveillance, XBB.1.5 accounted for 74.7% of infections, followed by BQ.1.1 at 16.3%, BQ.1 at 5.1%, XBB at 1.9%, CH.1.1 at 1.3%, BN.1 at 0.8%, BA.5 at 0.3%, and BF.7 at 0.3%.
BQ.1.1 has five spike mutations that are different from BA.5. Four of these mutations allow escape from immunity from monoclonal antibodies, any prior infection (including Omicron BA.5), or any vaccine to include the bivalent Omicron BA.5 vaccine. Infections are still occurring in our clinic in patients that received the Omicron BA.5 bivalent vaccine. The XBB recombinant isolate XBB.1.5 has rapidly become the dominant infection in the USA. It took 28 days to become the cause of 40% of infections in the USA. As of 1/14/23, XBB.1.5 now causes over 80% of infections in Regions 1 and 2.
The “Omicron family feud” is a phrase coined by Dr. Raj Rajnarayanan to describe what’s going on between the Omicron BQ variants, BQ.1, BQ,1.1 (and other BQ variants) and XBB.1.5 (and other XBB variants). In the USA in regions 1 and 2, XBB.1.5 has won the feud. A new variant of BA2.75, CH.1.1, is now 4.9% of SARS-CoV-2 isolates in the world. It has the Delta mutation, P681R, which should raise a red flag. According to Saito et al, the P681R mutation, “facilitates cleavage of the spike protein and enhances viral fusogenicity [the ability of the virus to fuse to human cell membranes]….and pathogenicity [lethality].”
XBB.1.5 Proportion of Sequenced Isolates in the USA
| 12/3/22 | 12/10/22 | 12/17/22 | 12/24/22 | 12/31/22 | 1/7/23 | 1/14/23 | 1/21/23 | 1/28/23 | 2/04/23 | 2/11/23 |
| 2.3% | 4.4% | 7.4% | 11.8% | 20.1% | 30.4% | 43.0% | 49.1% | 61.3% | 65.9% | 74.7% |
BQ. 1 and BQ.1.1 Totaled Proportion of Sequenced Isolates in the USA
| 12/3/22 | 12/10/22 | 12/17/22 | 12/24/22 | 12/31/22 | 1/7/23 | 1/14/23 | 1/21/23 | 1/28/23 | 2/04/23 | 2/11/23 |
| 53.5% | 57.4% | 58.6% | 60.3% | 59.2% | 53.2% | 44.7% | 40.2% | 31.1% | 27.4% | 21.4% |
Percent of isolates identified as XBB.1.5 by Region
| Region | ||||||||||
| Week ending in | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 |
| 12/31/22 | 75.3% | 72.2% | 32.7% | 19.0% | 6.0% | 21.5% | 8.1% | 2.1% | 9.2% | 2.5% |
| 1/14/23 | 81.7% | 82.7% | 49.0% | 31.1% | 14% | 24.9% | 8.8% | 15% | 15.8% | 8.1% |
| 1/28/23 | 89.3% | 91.1% | 72.5% | 52.1% | 36.5% | 42.8% | 24.4% | 32.5% | 35.1% | 20.3% |
| 2/11/23 | 93.8% | 95.2% | 85.8% | 72.4% | 60.4% | 63.4% | 53.1% | 60.9% | 56.9% | 37.4% |
SARS-CoV-2 infections per day in the United States have increased for the second time in 6 weeks. There is still widespread underreporting by states, a failure to capture all positive home tests, and a decreased PCR screening program in most states. Deaths per day in the United States have increased by 147 deaths per day. Many states are not reporting deaths or infections in a timely manner. The number of infections per day is expected to increase in the next four weeks due to a lack of mask use in schools, businesses, and airports; a failure of adequate building ventilation; lack of social distancing; and low rates of bivalent booster uptake. XBB, an Omicron recombinant variant first identified in India, caused a major outbreak in Singapore. XBB is the first recombinant variant combining spike protein sequences from two other Omicron BA.2 variants, that has spread aggressively around the world. New mutations of XBB, specifically XBB.1.5 have rapidly crowded out other variants in the USA. Current vaccines, monoclonal antibodies and prior infections will not protect you from getting an XBB.1.5 infection. A more detailed description of XBB variant mutations and epidemiology can be found on page 17 of the UK Health Security Agency Technical Briefing from November 25.
Troubling Variant News from the UK
The latest UK Health Security Agency Technical Briefing, published February 10, reports that variants XBB.1.5 and CH.1.1, along with their sublineages, have a growth advantage over previously dominant variants, are likely responsible for the current increase in cases in the UK, and “will continue to increase overall transmission as they become more prevalent.” In addition, they state that, based on their data, vaccine effectiveness against CH.1.1 and XBB.1.5 may be reduced compared to BQ.1. From this, we can conclude, as we have previously, that vaccination alone is not enough to protect people from being infected with these newer SARS-CoV-2 variants.
Another new variant, XBF, which is a recombinant of BA.5 and CJ.1 (which is a descendant of BA.2.75) has also shown up in low proportions in the UKHSA’s signal monitoring. More troubling is that, per GISAID, XBF currently accounts for more than 15% of sequences in Australia. We’ll be watching carefully to see which isolate will eventually supplant XBB.1.5. At this stage, it’s unclear whether it will be a mutation of XBB.1.5, another recombinant like XBF, or something else.
Yet another piece of bad news from UKHSA concerns molnupiravir, one of two oral antiviral medications approved in the U.S. for the treatment of COVID-19. This drug works by causing a large number of random mutations in the virus, which hinder its replication. That also means that molnupiravir leaves a particular “signature” of mutations that can be observed through viral sequencing. The Technical Briefing references a new preprint out of the London-based Francis Crick Institute which contains analysis of more than 13 million SARS-CoV-2 sequences in global databases. The researchers observed “a set of long phylogenetic branches that exhibit a high number of transition mutations.” In other words, on the SARS-CoV-2 family tree, there are some variants that are very different from their parents. They also observed that the number of these long branches (with more mutations between variant and sub-variant) increased in 2022, after the introduction of molnupiravir, and that the variants on those branches were more common in countries where molnupiravir was in use. In addition, they noted that the patterns of mutations among these variants were “highly similar to that in patients known to be treated with molnupiravir.” They conclude that there have been some cases in which “viruses with a large number of molnupiravir-induced substitutions have been transmitted to other individuals.” This analysis was compelling enough that the UKHSA’s Variant Technical Group is recommending further investigation into the impact of molnupiravir treatment on the evolution of the virus, especially in the case of chronic infections and infections in immunocompromised people.
In our clinic, we only treat patients with Paxlovid because of our concerns about the potential of developing new resistant variants on molnupiravir therapy, particularly in our immunocompromised patients. If additional information develops about the mutation problem with molnupiravir, then the drug may need to be pulled off the market.
For a more detailed picture of COVID variant evolution in the United States, we recommend checking out the dashboard put together by Raj Rajnarayanan, Assistant Dean of Research and Associate Professor at NYITCOM at Arkansas State University.
To understand the true impact of these variants, it’s helpful to examine their evolution. Two virologists collaborated on Twitter to create the figure below, which Professor Johnson titled “Convergent Evolution on Steroids.” It shows the key mutations present in many of the currently-circulating Omicron subvariants and demonstrates that mutation at site 346 is becoming more and more common.
Past infections with a BA.1, BA.2 or BA.5 variants will not prevent infections with any of the newer variants. Monoclonal antibodies are no longer effective against newer BQ variants, XBB variants and other spike protein mutated variants. The last remaining monoclonal antibody, bebtelovimab, was removed from use by the FDA on 12/2/22. Paxlovid was only 89% effective in the original clinical trials against SARS-CoV-2. If resistance develops this winter to oral Paxlovid, we will have more Paxlovid failures and increased hospitalizations and deaths.
A Deeper Dive into U.S. COVID Data
On 1/27/23, the United States had 12,107 documented new infections. There were also 159 deaths. Thirty-nine states did not report their infections, and 38 states and the District of Columbia didn’t report their deaths. In the United States on 2/09/23 the number of hospitalized patients (29,299) has decreased (-13.83% compared to the previous 14 days) and was 34,015 on January 27. On 1/27/23 there were 3,608 patients who were seriously or critically ill (a 17.03% decrease); that number was 4,349 two weeks ago. The number of critically ill patients has decreased by 741 in the last 14 days, while at least 7,743 new deaths occurred. Patients are still dying each day (average 553/day).
As of 2/10/23, we have had 1,139,979 deaths and 104,760,445 SARS-CoV-2 infections in the United States. We have had 653,533 new infections in the last 14 days. We are adding an average of 326,767 new infections every seven days. For the pandemic in the United States we are averaging one death for every 91.89 infections or over 10,882 deaths for each one million infections. As of 2//23, thirty-nine states have had greater than 500,000 total infections, and 38 states and Puerto Rico have had greater than 5,000 total deaths. Forty-six states have had greater than 2,000 deaths. Only Vermont has had less than a thousand deaths (901 deaths). Now 11 states have over 4,000 deaths per million population: Mississippi (4,444), Arizona (4,525), Alabama (4,261), West Virginia (4,410), New Mexico (4,293), Tennessee (4,234), Arkansas (4,281), Michigan (4,186), New Jersey (4,038), Kentucky (4,015) and Louisiana (4,006). Eighteen states (Alabama, Virginia, Missouri, North Carolina, Indiana, Tennessee, Massachusetts, Ohio, Michigan, Georgia, Illinois, New Jersey, Pennsylvania, Florida, Texas, New York, Arizona and California) have had greater than 20,000 deaths. Nine states have had greater than 40,000 deaths: Florida (85,710 deaths), Texas (93,364 deaths), New York (76,800 deaths), Pennsylvania (49,921 deaths), Georgia (42,161 deaths), Ohio (41,535 deaths), Illinois (41,263 deaths), Michigan (41,809), and California (100,345 deaths, 20th most deaths in the world).
On 11/20/20, there were 260,331 (cumulative) deaths in the US from SARS-CoV-2. Since 11/20/20 (27 months), there were 872,878 new deaths from SARS-CoV-2. For twenty-three of those months, vaccines have been available to all adults. During these twenty-three months, 567,780 people have died of SARS-CoV-2 infections. Clearly, a vaccine-only approach is not working anywhere, especially not in the United States. In addition to getting more people vaccinated, most of the hospitalizations and deaths could have been prevented by proper masking (N95 or better), social distancing, and treatment with oral antiviral agents like Paxlovid. We recommend all of these precautions and treatments to every patient in our clinic, and we have only lost one patient to COVID in 3 years.
As of 2/10/23, California was ranked 31st in the USA in infection percentage at 30.39%. In California, 26.42% of the people were infected in the last 22 months. As of 2/10/23, 33 states have had greater than 30% of their population infected. Fifty states, the District of Columbia and Puerto Rico have greater than 20% of their population infected.
Don’t want to miss an update?
Get the latest COVID updates from Dr. Wright delivered to your inbox as soon as they’re published!
FDA-Approved Oral Drug Treatments for SARS-CoV-2
Pfizer has developed PAXLOVID™, an oral reversible inhibitor of C3-like protease of SARS-CoV-2. The drug inhibits this key enzyme that is crucial for virus production. The compound, also called Compound 6 (PF-07321332), is part of the drug combination PAXLOVID™ (PF-07321332; ritonavir), which successfully completed a Phase 2-3 trial in humans in multiple countries. The preliminary results were announced on 11/5/21 by Pfizer. The results showed that 89% of the hospitalizations and deaths were prevented in the drug treatment arm. The drug was administered twice a day for five days. No deaths occurred in the treatment group, and ten deaths occurred in the placebo group. The study was stopped by an independent data safety monitoring board, and the FDA concurred with this decision. Pfizer applied for an Emergency Use Authorization for this drug on 11/15/21. This drug was approved on 12/23/21. PAXLOVID™ one year later is widely available at major pharmaceutical chains and smaller independent drug stores throughout the USA. We have been able to obtain PAXLOVID™ for any patient desiring treatment. We have only had one drug failure and death from SARS-CoV-2 during 2022. That death occurred in an octogenarian male in the fourth quarter of 2022.
Watching World Data
Over the next few months, we’ll be paying close attention to correlations between the SARS-CoV-2 data, the number of isolates identified in various countries and states, and the non-pharmaceutical interventions (like mask mandates and lockdowns) put in place by state and national governments. Data on infections, deaths, and percent of population infected was compiled from Worldometers. Data for this table for SARS-CoV-2 Isolates Currently Known in Location was compiled from GISAID and the CDC. It’s worth noting that GISAID provided more data than the CDC.
| Location | Total Infections as of 2/10/23 | New Infections on 2/10/23 | Total Deaths | New Deaths on 2/10/23 | % of Pop.Infected | SARS-CoV-2 Isolates Currently Known in Location | National/ State Mask Mandate | Currently in Lockdown |
| World | 677,294,111(2,779,648 new infections in the last 14 days with an average of 198,546 infections per day). | 135,509 | 6,780755(52,474 new deaths in the last 14 days with an average of 3,748 deaths per day.) | 888 | 8.68% | B2 lineageAlpha/B.1.1.7 (UK)Eta/B.1.525 (Nigeria/UK)Iota/B.1.526 (USA-NYC)Beta/B.1.351 (SA)Epsilon/B.1.427 + B.1.429 (USA)*Gamma/P.1 (Brazil)Zeta/P.2 (Brazil)A lineage isolateV01.V2 (Tanzania)APTK India VOC 32421Delta/B.1.617.2 (India)BV-1 (Texas, USA)Kappa/B.1.617.1 (India)Lambda/C.37 (Peru)Theta/P.3 (Philippines) Mu/B.1.621 (Colombia)C.1.2 (South Africa 2% of isolates in July 2021)R1 (Japan)Omicron/B.1.1.529 + BA.1 + BA.2 + BA.3 (South Africa November 2021)B.1.640.1 (Congo/France)B.1.640.2 (Cameroon/France)Four new recombinants 12/31 to 3/22)BA.2.12.1 (USA)BA.4 (South Africa)BA.5 (South Africa)BA.2.75 (India 7/22)BA.4.6 (USA 7/22)BF.7BJ.1XBB (new recombinant India)BQ.1BQ.1.1BS.1BN.1XBB.1XBB.1.5CH.1.1 | No | No |
| USA | 104,760,445(ranked #1) 653,533 new infections in the last 14 days with an average of 46,681 infections/day | 12,107(ranked #7) 39 states failed to report infections on 2/10/23. | 1,139,979(ranked #1) 7,743 new deaths reported in the last 14 days or an average of 553 deaths/ day. | 159 38 states failed to report deaths on 2/10/23. | 31.29% | B2 lineageAlpha/B.1.1.7 (UK)Eta/B.1.525 (Nigeria/UK)Iota/B.1.526 (USA-NYC)Beta/B.1.351 (SA)Epsilon/B.1.427 + B.1.429 (USA)*Gamma/P.1 (Brazil)Zeta/P.2 (Brazil)Delta/B.1.617.2 (India)BV-1 (Texas, USA)Theta/P.3 (Philippines) Theta/P.3 (Philippines) Kappa/B.1.617.1 (India)Lambda/C.37 (Peru)Mu/B.1.621 (Colombia)R1(Japan) Omicron/B.1.1.529 + BA.1 + BA.2 (South Africa November 2021)B.1.640.1 (Congo/France)Recombinant Delta AY.119.2- Omicron BA.1.1 (Tennessee, USA 12/31/21)\BA.2BA.2.12.1 (United States)BA.4 (South Africa 11/21)BA.5 (South Africa 11/21)BA.2.75 (India 7/22)BA.4.6 (USA 7/22)BA.4.6 (USA 7/22)BF.7BJ.1XBB (new recombinant India)BQ.1BQ.1.1BN.1XBB.1XBB.1.5CH.1.1 | No | No |
| Brazil | 36,930,339(ranked #5) 124,372 new infections in the last 14 days. | 12,716 (ranked#5) | 697,662(ranked #2; 1,777 new deaths in the last 14 days) | 42 | 17.14% | No | No | |
| India | 44,682,530(ranked #2). | – | 530,739(ranked #3) | – | 3.17% Unchanged in 8 weeks | No | No | |
| United Kingdom | 24,293,752(ranked #9) 34,506 new infections in the last 2 weeks. | – | 204,898 (ranked #7) 1,669 new deaths in the last 2 weeks | – | 35.46% | B2 lineageAlpha/B.1.1.7 (UK)Eta/B.1.525 (Nigeria/UK)Beta/B.1.351 (SA)Epsilon/B.1.427 + B.1.429 (USA)*Gamma/P.1 (Brazil)Delta/B.1.617.2 (India)Theta/P.3 (Philippines) Kappa/B.1.617.1 (India)Lambda/C.37 (Peru)Mu/B.1.621 (Colombia)C.1.2 (South Africa)Omicron/B.1.1.529 + BA.1 (South Africa November 2021)B.1.640.1 (Congo/France)XD (AY.4/BA.1) recombinantXF (Delta/BA.1) recombinantXE (BA.1/BA.2) recombinantBA.2BA.2.12.1 (United States)BA.4 (South Africa 11/21)BA.5 (South Africa 11/21)BA.2.75 (India 7/22) | No | No |
| California, USA | 12,011,521(ranked #12 in the world; 50,447 new infections in the last 14 days). | 1,459 | 100,345 (ranked #20 in world; 452 new deaths in the last 14 days | 22 | 30.39% | B2 lineageAlpha/B.1.1.7 (UK)Eta/B.1.525 (Nigeria/UK)Beta/B.1.351 (SA)Gamma/P.1 (Brazil)Epsilon/B.1.427 + B.1.429 (USA)*Zeta/P.2 (Brazil)Delta/B.1.617.2 (India)Theta/P.3 (Philippines) Kappa/B.1.617.1 (India)Lambda/C.37 (Peru) Mu/B.1.621 (Colombia) Omicron/B.1.1.529 + BA.1 (South Africa November 2021)BA.2BA.2.12.1 (United States)BA.4 (South Africa 11/21)BA.5 (South Africa 11/21)BA.2.75 (India 7/22)BQ.1BQ.1.1BN.1XBBXBB.1XBB.1.5CH.1.1 | No | No |
| Mexico | 7,400,848(ranked #19) 47,218 new infections in 14 days). | – | 332,850(ranked #5) 834 new deaths in the last 14 days) | – | 5.62% | No | No | |
| South Africa | 4,057,211(ranked #38; 1,927 new infections in the last 14 days). | – | 102,595 (ranked #18) no new deaths in the last 14 days). | – | 6.67% | B2 lineageAlpha/B.1.1.7 (UK)Beta/B.1.351 (SA)Delta/B.1.617.2 (India)Kappa/B.1.617.1 (India) C.1.2 (South Africa, July 2021)Omicron/B.1.1.529 + BA.1 (South Africa November 2021)B.1.640.1 (Congo/France)BA.2BA.4 (South Africa 11/21)BA.5 (South Africa 11/21) | No | No |
| Canada | 4,560,962(ranked #34) 21,733 new infections in 14 days). | – | 50,629(ranked #24) 494 new deaths in the last 14 days. | – | 11.88% | No | No | |
| Russia | 22,047,525 (ranked #10), 77,539 new infections in 14 days). | 12,392 (ranked #6) | 395,484(ranked #4)582 new deaths in 14 days | 37 | 15.12% | No | No | |
| Peru | 4,483,236(ranked #35, 2,408 new infections in 14 days). | 200 | 219,229(ranked #6) 500 new deaths in the last 14 days. | 1 | 13.31% | No | No | |
| Spain | 13,748,918(ranked #12; 37,667 new infections in 14 days). | 1,119 (ranked #13) | 118,876 (ranked #16) 542 new deaths in 14 days. | 36 | 29.42% | No | No | |
| France | 39,,559,127 (ranked #3) | 3,336 (ranked #9) | 164,537 (ranked #10) 457 new deaths in 14 days. | 44 | 60.31% a 0.07% increase in 14 days. | No | No | |
| Germany | 37,739,472(ranked #4; 167,840 new infections in 14 days.) | 13,420 (ranked #4) | 166,763 (ranked #9)1,322 new deaths in 14 days. | 103 | 45.19%0.20% increase in 14 days | No | No | |
| South Korea | 30,325,483 (ranked #7; 218,129 new infections in 14 days). | 13,504(ranked #3) | 33,697 (ranked #34) 365 new deaths in 14 days. | 17 | 59.07%0.42% increase in 14 days | No | No | |
| Netherlands | 8,586,372 (ranked #17; 4,951 new infections in 14 days). | 396 | 22,992 (ranked #41) | – | 49.88% | No | No | |
| Taiwan | 9,773,627(ranked #16); 345,147 new infections in 14 days | 16,964 (ranked #2) | 16,964 (ranked #56; 760 new deaths in the last 14 days) | 70 | 40.91% 1.45% of population has been infected in the last 14 days | No | No | |
| Japan | 32,908,240(ranked #6)543,390 new infections in the last 14 days | 28,615(ranked #1) | 70,377(ranked #20) 3,327 new deaths in the last 14 days for an average of 238 deaths per day. | 192 | 26.20% 0.43-% of the population infected in the last 14 days. | No | No | |
| Australia | 11,330,342(ranked #14) 34,876 new infections in 14 days. | 2,491 (ranked #10) | 19,070(ranked #49) 455 new deaths in 14 days. | 35 | 43.46% 0.14-% of the population infected in last 14 days. | No | No | |
| Hong Kong | 2,880,518(ranked# 41) 62,811 new infections in the last 14 days. | 250 | 13,412 (ranked#60)132 new deaths in the last 14 days. | 5 | 37.88% 0.15% of the population infected in the last 14 days. | No | No | |
| China | 503,302 | – | – | – | – | – | – | – |
What Our Team Is Reading This Week
- SARS-CoV-2 variants of concern and variants under investigation in England Technical briefing 50, 10 February 2023 https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1135877/variant-technical-briefing-50-10-february-2023.pdf
- Identification of a molnupiravir-associated mutational signature in SARS-CoV-2 sequencing databases (Preprint) https://doi.org/10.1101/2023.01.26.23284998
- COVID drug drives viral mutations — and now some want to halt its use https://www.nature.com/articles/d41586-023-00347-z#ref-CR1
- SARS-CoV-2 variants of concern and variants under investigation in England Technical briefing 49, 11 January 2023 https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1128554/variant-technical-briefing-49-11-january-2023.pdf
- Long COVID: major findings, mechanisms and recommendations (Nature) https://www.nature.com/articles/s41579-022-00846-2
- Enhanced fusogenicity and pathogenicity of SARS-CoV-2 Delta P681R mutation (Nature) https://doi.org/10.1038/s41586-021-04266-9
- Virological characteristics of the SARS-CoV-2 XBB variant derived from recombination of two Omicron subvariants (Preprint) https://doi.org/10.1101/2022.12.27.521986
- SARS-CoV-2 infection and persistence in the human body and brain at autopsy (Nature) https://doi.org/10.1038/s41586-022-05542-y
- Lifting Universal Masking in Schools — Covid-19 Incidence among Students and Staff (NEJM) https://www.nejm.org/doi/full/10.1056/NEJMoa2211029
- FDA Announces Bebtelovimab is Not Currently Authorized in Any US Region (FDA) https://www.fda.gov/drugs/drug-safety-and-availability/fda-announces-bebtelovimab-not-currently-authorized-any-us-region
- SARS-CoV-2 variants of concern and variants under investigation in England Technical briefing 48, 25 November 2022 (UK Health Security Agency) https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1120304/technical-briefing-48-25-november-2022-final.pdf
- Omicron sublineage BQ.1.1 resistance to monoclonal antibodies (The Lancet) https://doi.org/10.1016/S1473-3099(22)00733-2
- SARS-CoV-2 Infection and Increased Risk for Pediatric Stroke (Pediatric Neurology) https://www.pedneur.com/article/S0887-8994(22)00210-7/fulltext
- Single-cell multiomics revealed the dynamics of antigen presentation, immune response and T cell activation in the COVID-19 positive and recovered individuals https://doi.org/10.3389/fimmu.2022.1034159
- Novel treatment combining antiviral and neutralizing antibody-based therapies with monitoring of spike-specific antibody and viral load for immunocompromised patients with persistent COVID-19 infection (Experimental Hematology & Oncology) https://ehoonline.biomedcentral.com/articles/10.1186/s40164-022-00307-9
- Covid-19 is a leading cause of death in children and young people ages 0-19 years in the United States (Preprint) https://doi.org/10.1101/2022.05.23.22275458
- Post-COVID-19-associated morbidity in children, adolescents, and adults: A matched cohort study including more than 157,000 individuals with COVID-19 in Germany (PLOS Medicine) https://journals.plos.org/plosmedicine/article?id=10.1371%2Fjournal.pmed.1004122
- Endothelial dysfunction in COVID-19: an overview of evidence, biomarkers, mechanisms and potential therapies (Acta Pharmacologica Sinica) https://doi.org/10.1038/s41401-022-00998-0
- Cognitive Deficits in Long Covid-19 (NEJM) https://www.nejm.org/doi/full/10.1056/NEJMcibr2210069
- Brain 18F-FDG PET imaging in outpatients with post-COVID-19 conditions: findings and associations with clinical characteristics (European Journal of Nuclear Medicine and Molecular Imaging) https://doi.org/10.1007/s00259-022-06013-2
- Acute and postacute sequelae associated with SARS-CoV-2 reinfection (Nature) https://doi.org/10.1038/s41591-022-02051-3
- Associations between indoor relative humidity and global COVID-19 outcomes (Journal of the Royal Society) https://doi.org/10.1098/rsif.2021.0865
- Successful treatment of prolonged, severe COVID-19 lower respiratory tract disease in a B-cell ALL patient with an extended course of remdesivir and nirmatrelvir/ritonavir (Clinical Infectious Diseases) https://doi.org/10.1093/cid/ciac868
- Impact of SARS-CoV-2 ORF6 and its variant polymorphisms on host responses and viral pathogenesis (Preprint) https://doi.org/10.1101/2022.10.18.512708
- Anti-PF4 antibodies associated with disease severity in COVID-19 (PNAS) https://www.pnas.org/doi/10.1073/pnas.2213361119
- A multinational Delphi consensus to end the COVID-19 public health threat (Nature) https://doi.org/10.1038/s41586-022-05398-2
- Pfizer and BioNTech Announce Updated Clinical Data for Omicron BA.4/BA.5-Adapted Bivalent Booster Demonstrating Substantially Higher Immune Response in Adults Compared to the Original COVID-19 Vaccine https://www.pfizer.com/news/press-release/press-release-detail/pfizer-and-biontech-announce-updated-clinical-data-omicron
- Paxlovid and Long Covid (Ground Truths, Eric Topol) https://erictopol.substack.com/p/paxlovid-and-long-covid?utm_source=substack&utm_medium=email
- Risk of Infection and Hospitalization Among Children and Adolescents in New York After Emergence of the SARS-CoV-2 Omicron Variant – Comment and Response (JAMA) https://jamanetwork.com/journals/jama/article-abstract/2797231
- Myocarditis (NEJM) https://www.nejm.org/doi/full/10.1056/NEJMra2114478
- SARS-CoV-2 variants of concern and variants under investigation in England Technical briefing 47 (UK Health Security Agency) https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/1115077/Technical-Briefing-47.pdf
- Effectiveness of Monovalent mRNA Vaccines Against COVID-19–Associated Hospitalization Among Immunocompetent Adults During BA.1/BA.2 and BA.4/BA.5 Predominant Periods of SARS-CoV-2 Omicron Variant in the United States — IVY Network, 18 States, December 26, 2021–August 31, 2022 (MMWR) https://www.cdc.gov/mmwr/volumes/71/wr/mm7142a3.htm
- “Three-dose monovalent mRNA VE estimates against COVID-19–associated hospitalization decreased with time since vaccination. Three-dose VE during the BA.1/BA.2 and BA.4/BA.5 periods was 79% and 60%, respectively, during the initial 120 days after the third dose and decreased to 41% and 29%, respectively, after 120 days from vaccination.”
- Saliva antibody-fingerprint of reactivated latent viruses after mild/asymptomatic COVID-19 is unique in patients with myalgic-encephalomyelitis/chronic fatigue syndrome (Frontiers in Immunology) https://doi.org/10.3389/fimmu.2022.949787
- SARS-CoV-2 Nsp6 causes cardiac defects through MGA/MAX complex-mediated increased glycolysis (Preprint) https://doi.org/10.21203/rs.3.rs-1677754/v1
















You must be logged in to post a comment.